- Understanding the Progression
- Stage 1: Simple Fatty Liver (Steatosis)
- Stage 2: Non-Alcoholic Steatohepatitis (NASH)
- Stage 3: Fibrosis (Scarring)
- Stage 4: Cirrhosis (Advanced Scarring)
- Understanding Fatty Liver Stages and Progression Rates
- How Doctors Determine Your Stage
- What You Can Do at Each Stage
- The Importance of Early Detection
- Moving Forward with Hope
When you’re told you have fatty liver disease, one of the first things you’ll want to know is how serious it is. Fatty liver disease isn’t just one condition—it’s a spectrum that ranges from mild and easily reversible to severe and life-threatening. Understanding which stage you’re at can help you grasp what’s happening in your body and what steps you need to take.
Let’s walk through each stage of fatty liver disease, what happens at each level, and what it means for your health.
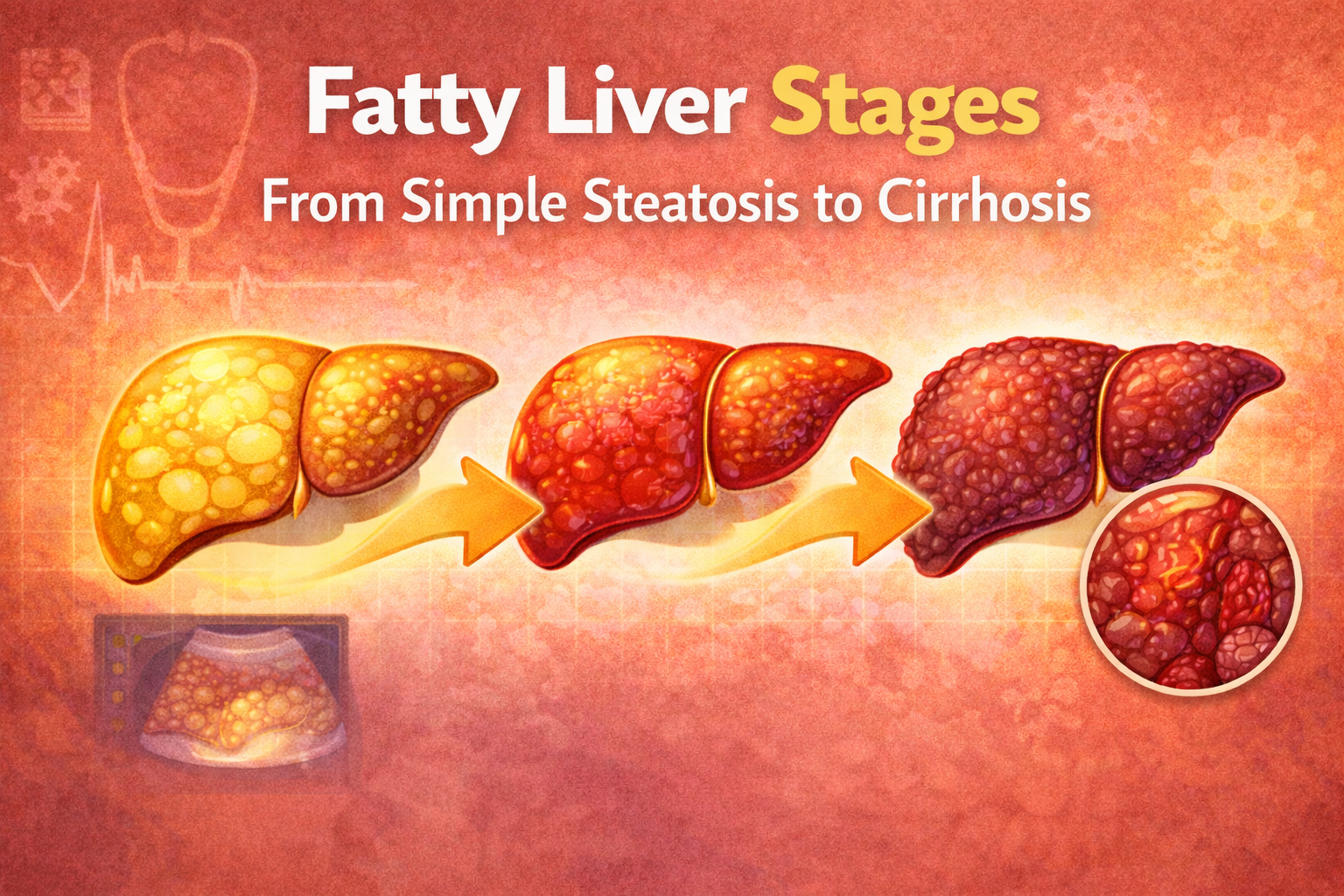
Understanding the Progression
Fatty liver disease doesn’t usually jump from mild to severe overnight. It typically progresses through distinct stages over months, years, or even decades. The good news is that progression isn’t inevitable. Many people stay at early stages their entire lives, and with the right changes, you can even move backward through the stages.
Think of it like a warning system. The early stages are your body’s way of saying “something needs to change.” The later stages are more urgent alarms. The key is catching it early and taking action before permanent damage occurs.
Not everyone progresses through all stages. Some people remain at stage one indefinitely. Others may progress more quickly, especially if they have additional risk factors like diabetes, obesity, or continue unhealthy habits. Your genetics, lifestyle, and overall health all play a role in determining how fatty liver disease affects you personally.
Stage 1: Simple Fatty Liver (Steatosis)
The first stage is called simple fatty liver or steatosis. This is where excess fat accumulates in your liver cells, but there’s no inflammation or cell damage yet. If your liver were a storage unit, this stage is like having too much stuff crammed in, but nothing is broken or damaged.
At this stage, your liver still functions normally. Most people have absolutely no symptoms. You feel fine, have normal energy levels, and wouldn’t know anything was wrong without testing. In fact, many people discover they have simple fatty liver by accident during routine blood work or imaging tests done for other reasons.
The amount of fat can vary. Doctors consider it fatty liver when more than 5% of your liver’s weight is fat. In simple steatosis, you might have anywhere from 5% to 30% or more fat content, but without inflammation.
This is the best stage to catch fatty liver disease because it’s almost always reversible. With weight loss, dietary changes, and exercise, most people can clear the excess fat from their liver within months to a year. Your liver has an amazing ability to heal itself at this stage.
Blood tests might show slightly elevated liver enzymes, but often they’re completely normal. An ultrasound or other imaging might show a “bright liver” or increased echogenicity, which indicates fat accumulation. Sometimes a FibroScan, a special test that measures liver stiffness and fat content, is used to assess the severity.
Stage 2: Non-Alcoholic Steatohepatitis (NASH)
The second stage is where things get more serious. NASH stands for non-alcoholic steatohepatitis, which is basically fatty liver with inflammation. The “itis” at the end means inflammation, just like arthritis means joint inflammation.
At this stage, the accumulated fat has triggered an inflammatory response. Your immune system recognizes that something is wrong and sends inflammatory signals to the liver. This inflammation starts to damage liver cells. It’s like that overstuffed storage unit caught fire—now there’s actual damage happening, not just overcrowding.
Some people with NASH start experiencing symptoms, though many still feel fine. When symptoms do occur, they’re usually vague and easy to dismiss. You might feel unusually tired, especially in the afternoon. Some people notice a dull ache in their upper right abdomen where the liver sits. Others just feel generally unwell without being able to pinpoint why.
Blood tests at this stage typically show elevated liver enzymes, particularly ALT and AST. These enzymes leak out of damaged liver cells into your bloodstream, so higher levels indicate more cell damage. However, normal enzyme levels don’t rule out NASH—you can have inflammation even with normal blood work.
NASH is significant because it’s the stage where liver damage begins. While still potentially reversible with aggressive lifestyle changes, it requires more effort and commitment than simple fatty liver. Studies show that people with NASH who lose 10% or more of their body weight can often reverse the inflammation and return to simple fatty liver or even normal liver.
About 20-30% of people with simple fatty liver will progress to NASH over time. Having diabetes, obesity, high blood pressure, or high cholesterol increases your risk of progression. The longer fatty liver goes untreated, the higher the chance of moving to this inflammatory stage.
Stage 3: Fibrosis (Scarring)
When inflammation persists in your liver, scar tissue begins to form. This stage is called fibrosis. Think of it like how your skin forms a scar after a deep cut—your liver does the same thing in response to ongoing damage.
Fibrosis is graded on a scale, typically from F0 (no fibrosis) to F4 (cirrhosis, which we’ll discuss next). Stages F1 through F3 represent increasing amounts of scar tissue. In early fibrosis (F1), there’s minimal scarring. As it progresses to F2 and F3, more and more healthy liver tissue is replaced by scar tissue.
The problem with scar tissue is that it doesn’t function like normal liver tissue. Scars can’t filter your blood, make proteins, or perform the hundreds of other jobs your liver does. As scar tissue increases, your liver’s ability to do its work decreases.
Most people with early to moderate fibrosis still don’t have obvious symptoms. Your liver has remarkable reserve capacity—it can function fairly well even when partially scarred. Symptoms, when they appear, are similar to NASH: fatigue, abdominal discomfort, and general malaise.
Diagnosing fibrosis usually requires specialized testing. A FibroScan can estimate the degree of scarring. Sometimes doctors use blood tests that calculate a fibrosis score based on various markers. A liver biopsy, where a small sample of liver tissue is examined under a microscope, is the gold standard for staging fibrosis, though it’s invasive and not always necessary.
The reversibility of fibrosis is debated, but research suggests that early-stage fibrosis (F1-F2) can improve with weight loss and lifestyle changes. More advanced fibrosis (F3) is harder to reverse, but progression can usually be stopped or slowed significantly. The key is aggressive intervention before reaching the final stage.
Stage 4: Cirrhosis (Advanced Scarring)
Cirrhosis is the most advanced stage of fatty liver disease, where extensive scarring has replaced much of the normal liver tissue. At this point, the damage is generally considered permanent. The liver’s structure is distorted, and its function is significantly impaired.
There are two types of cirrhosis: compensated and decompensated. In compensated cirrhosis, your liver still manages to do most of its jobs despite the scarring. You might have few or no symptoms. In decompensated cirrhosis, your liver can no longer keep up with its workload, and serious complications develop.
Symptoms of cirrhosis can include persistent fatigue, easy bruising and bleeding, swelling in your legs and abdomen, yellowing of the skin and eyes (jaundice), confusion or mental fogginess, and loss of appetite and weight. Some people develop spider-like blood vessels on their skin or reddening of the palms.
Cirrhosis can lead to life-threatening complications. Portal hypertension, or high blood pressure in the veins leading to the liver, can cause dangerous bleeding from enlarged veins in the esophagus or stomach. Fluid can accumulate in the abdomen (ascites) or around the lungs. The brain can be affected by toxins the liver can no longer filter out, causing confusion or even coma.
People with cirrhosis also have an increased risk of liver cancer. Once cirrhosis develops from fatty liver disease, the annual risk of liver cancer is about 1-3%. This is why regular monitoring with ultrasound and blood tests becomes crucial at this stage.
While cirrhosis itself can’t be reversed, lifestyle changes are still important. They can prevent further damage, reduce the risk of complications, and improve quality of life. In cases of decompensated cirrhosis, liver transplantation may become necessary. In fact, fatty liver disease has become one of the leading reasons people need liver transplants.
Understanding Fatty Liver Stages and Progression Rates
Not everyone progresses through these stages, and the timeline varies dramatically from person to person. Some people remain at simple fatty liver for decades without ever developing inflammation. Others progress more rapidly.
Several factors influence how quickly fatty liver disease progresses. Having diabetes significantly increases the risk and speed of progression. People with poorly controlled blood sugar are more likely to develop NASH and fibrosis. Obesity, particularly excess belly fat, accelerates progression. The more overweight you are and the longer you remain overweight, the greater your risk.
Age plays a role too. The liver’s ability to repair itself decreases as we get older, so progression may be faster in older adults. Genetics also matter—some people are simply more susceptible to developing severe liver disease than others.
Drinking alcohol, even in moderate amounts, can accelerate the progression of fatty liver disease. If you have fatty liver, even occasional drinking adds additional stress to your liver and increases inflammation. Complete alcohol avoidance is usually recommended.
On average, it can take 10-20 years or more to progress from simple fatty liver to cirrhosis, but this timeline is highly variable. Some people never progress at all, while others move through stages more quickly, particularly if they have multiple risk factors.
How Doctors Determine Your Stage
Figuring out which stage of fatty liver disease you’re at requires various tests. Blood tests measuring liver enzymes, blood sugar, cholesterol, and other markers provide important clues. Elevated ALT and AST suggest inflammation, while other markers can indicate fibrosis.
Imaging tests like ultrasound, CT scans, or MRI can show fat in the liver and sometimes detect scarring. A FibroScan is particularly useful because it measures both liver fat content and stiffness, which correlates with fibrosis.
Liver biopsy remains the most accurate way to stage fatty liver disease. A doctor removes a tiny piece of liver tissue with a needle, and a pathologist examines it under a microscope. This can definitively show the amount of fat, inflammation, and fibrosis. However, because it’s invasive and carries small risks, biopsies are typically reserved for cases where the diagnosis is unclear or when knowing the exact stage will significantly impact treatment decisions.
What You Can Do at Each Stage
No matter what stage you’re at, lifestyle changes make a difference. At the simple fatty liver stage, losing 5-10% of your body weight through diet and exercise can often completely reverse the condition. Focus on a balanced diet with plenty of vegetables, whole grains, lean proteins, and healthy fats while cutting out sugary drinks and processed foods.
If you have NASH, more aggressive intervention is needed. Aim for 10% or more weight loss. Regular exercise, at least 150 minutes per week of moderate activity, helps reduce inflammation. Work closely with your doctor to manage any related conditions like diabetes or high cholesterol.
For fibrosis, the goals are similar but the urgency is greater. Preventing progression to cirrhosis becomes critical. Some doctors may recommend medications to help control blood sugar or cholesterol more aggressively. Regular monitoring every 6-12 months helps catch any worsening early.
With cirrhosis, preventing complications becomes paramount. You’ll need regular screening for liver cancer and monitoring for signs of liver decompensation. Your doctor may prescribe medications to prevent bleeding or reduce fluid buildup. In some cases, referral to a transplant center for evaluation is appropriate.
The Importance of Early Detection
The progression through fatty liver stages underscores why early detection matters so much. Catching fatty liver disease at the simple steatosis stage gives you the best chance of complete reversal. Even at the NASH or early fibrosis stage, significant improvement is possible.
If you have risk factors like obesity, diabetes, high cholesterol, or a family history of liver disease, talk to your doctor about screening. Simple blood tests and an ultrasound can detect fatty liver before symptoms appear. The earlier you know, the more you can do to prevent progression.
Moving Forward with Hope
Understanding the stages of fatty liver disease can feel overwhelming, but knowledge is power. Knowing where you are on this spectrum helps you understand what actions to take and how urgent they are. The good news is that at every stage except advanced cirrhosis, positive changes can make a real difference.
Your liver is a remarkably resilient organ with an impressive ability to heal when given the chance. Whether you’re at stage one or stage three, taking steps toward a healthier lifestyle can stop progression, improve your liver function, and enhance your overall quality of life. The journey through fatty liver stages doesn’t have to be one-way—with commitment and the right support, you can move in the direction of better health.