If you’ve recently been diagnosed with fatty liver disease, or you’re worried because it runs in your family, you’re probably wondering whether your genes play a role. It’s a question I hear all the time, and honestly, the answer isn’t a simple yes or no. Let’s break down what we know about fatty liver disease, genetics, and what really affects your risk.
What Exactly Is Fatty Liver Disease?
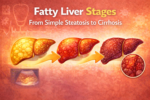
Before we talk about genetics, let’s make sure we’re on the same page about what fatty liver disease actually is. Your liver naturally contains some fat, but when fat makes up more than 5-10% of your liver’s weight, doctors call it fatty liver disease.
There are two main types. The first is alcoholic fatty liver disease, which develops from heavy drinking over time. The second is non-alcoholic fatty liver disease, or NAFLD, which happens in people who drink little to no alcohol. NAFLD is surprisingly common and affects about 25% of adults worldwide.

The tricky thing about fatty liver is that most people don’t have any symptoms in the early stages. You might feel tired or have some discomfort in your upper right abdomen, but many people don’t notice anything wrong until the condition progresses.
So, Is It Actually Genetic?
Here’s where things get interesting. Fatty liver disease isn’t inherited the same way something like eye color is. You don’t get a “fatty liver gene” from your parents that guarantees you’ll develop the condition. Instead, genetics influence your risk, sometimes quite significantly.
Research shows that if your parents or siblings have fatty liver disease, you’re more likely to develop it too. Studies have found that genetics account for roughly 20-30% of the variation in who gets fatty liver disease. That’s substantial, but it also means that 70-80% comes down to other factors you can actually control.
Scientists have identified several gene variants that increase susceptibility to fatty liver. The most well-studied is called PNPLA3. People with certain variations of this gene have a harder time breaking down fat in the liver, which leads to fat accumulation. Another gene, TM6SF2, affects how the liver processes and exports fat. If you have variations in these genes, your risk goes up.
But here’s the thing that many people find reassuring: having these genetic variants doesn’t mean you’ll definitely get fatty liver disease. It just means you need to be more careful about the lifestyle factors that contribute to it.
Why Fatty Liver Runs in Families
When fatty liver disease shows up in multiple family members, it’s often a combination of shared genes and shared habits. Think about it. Families usually eat similar foods, have similar activity levels, and may face similar stressors. If your family meals tend to be high in sugar and processed foods, or if everyone leads a pretty sedentary lifestyle, that environment affects everyone.
This is actually good news because it means you have power to change your risk, even if you have a genetic predisposition.
The Risk Factors You Can’t Change
Let’s be honest about the factors you’re stuck with:
Your ancestry matters. Hispanic and Asian populations have higher rates of fatty liver disease compared to other ethnic groups. If you’re of Hispanic descent, you’re about 1.5 times more likely to develop NAFLD. People of Asian descent can develop fatty liver at lower body weights than other populations.
Age plays a role too. While fatty liver can happen at any age, including in children, it becomes more common as you get older. Most cases are diagnosed in people between 40 and 60 years old.
Your gender influences risk in complex ways. Before menopause, women have lower rates of fatty liver than men. But after menopause, women’s risk increases and can even surpass men’s in some age groups.
The Risk Factors You CAN Change
Now for the empowering part. Most of the major risk factors for fatty liver disease are within your control. Let’s talk about what really matters.

Weight is the big one. About 70% of people with obesity have fatty liver disease. But here’s something important: you don’t have to be overweight to develop it. About 10-20% of people with normal weight have NAFLD, especially if fat tends to accumulate around their middle.
Type 2 diabetes and insulin resistance are huge risk factors. When your body becomes resistant to insulin, it struggles to regulate blood sugar and fat storage. This often leads to fat building up in the liver. If you have diabetes, your risk of fatty liver is much higher.
High cholesterol and triglycerides go hand in hand with fatty liver. Many people with fatty liver have what doctors call metabolic syndrome, which includes high blood pressure, high blood sugar, excess abdominal fat, and abnormal cholesterol levels.
What you eat matters tremendously. Diets high in refined carbohydrates, sugar, and processed foods increase your risk. That daily soda habit, those sugary coffee drinks, all that white bread and pasta, they all contribute. Fructose, especially from high-fructose corn syrup, is particularly problematic for the liver.
Being inactive is a major contributor. Regular exercise helps your body use insulin better and reduces fat in the liver. Even without weight loss, physical activity can improve fatty liver.
Understanding Your Personal Risk
So how do you figure out your own risk? Start by looking at your family history. Do any of your close relatives have fatty liver disease, diabetes, or metabolic syndrome? That’s a clue that you might have some genetic susceptibility.
Next, honestly assess your lifestyle. How’s your diet? Do you eat a lot of processed foods and sugar? How much do you move during the day? What’s your weight, particularly around your middle?
Get regular checkups. Blood tests can show elevated liver enzymes, though normal enzyme levels don’t rule out fatty liver. Your doctor might recommend an ultrasound or other imaging if you have risk factors.
What You Can Do Starting Today
The beautiful thing about fatty liver is that it’s often reversible, especially in the early stages. Here’s what actually works:
Start with your diet. You don’t need a complicated meal plan. Focus on whole foods: vegetables, fruits, whole grains, lean proteins, and healthy fats. Cut back on sugar, especially from drinks. Reduce processed foods. The Mediterranean diet has good research backing its benefits for liver health.
Move your body regularly. Aim for at least 150 minutes of moderate activity each week. That could be brisk walking, swimming, cycling, whatever you enjoy. Resistance training helps too. The key is consistency.
Lose some weight if you’re carrying extra pounds. Even a 5-10% reduction in body weight can significantly improve fatty liver. You don’t need to reach an “ideal” weight to see benefits.
Manage other health conditions. Keep your blood sugar, cholesterol, and blood pressure under control. These all affect your liver health.
Limit alcohol. Even if you have non-alcoholic fatty liver disease, alcohol can make it worse.
Be cautious with medications and supplements. Some can stress your liver. Always tell your doctor about everything you’re taking.
The Bottom Line
Is fatty liver disease genetic? Yes, partially. Genetics load the gun, but lifestyle pulls the trigger. If you have a family history of fatty liver, you’re not doomed to get it. And if you don’t have a family history, you’re not off the hook either.
The most important thing to understand is that you have more control than you might think. Your genes might make you more susceptible, but your daily choices, what you eat, how much you move, how you manage stress, these things have a powerful impact on whether you develop fatty liver disease and how severe it becomes.
If you’re concerned about your risk, talk to your doctor. Get tested if you have risk factors. And most importantly, start making small changes today. Your liver is remarkably good at healing itself when you give it what it needs: good nutrition, regular movement, and healthy habits.
Remember, understanding your risk isn’t about fear or fatalism. It’s about empowerment. It’s about taking the information and using it to make better choices for your health. And that’s something everyone can do, regardless of what’s written in their genes.