- Understanding Fatty Liver Disease
- The Two Main Types of Fatty Liver Disease
- What Causes Fatty Liver Disease?
- Recognizing the Symptoms
- How is Fatty Liver Disease Diagnosed?
- The Progression of Fatty Liver Disease
- Treatment and Management
- Prevention: Your Best Defense
- When to See a Doctor
- Living with Fatty Liver Disease
Fatty liver disease has become one of the most common liver conditions worldwide, affecting millions of people across all age groups. Despite its prevalence, many people remain unaware of this silent condition until it progresses to more serious stages. This comprehensive guide will help you understand what fatty liver disease is, its causes, symptoms, diagnosis, and most importantly, what you can do about it.
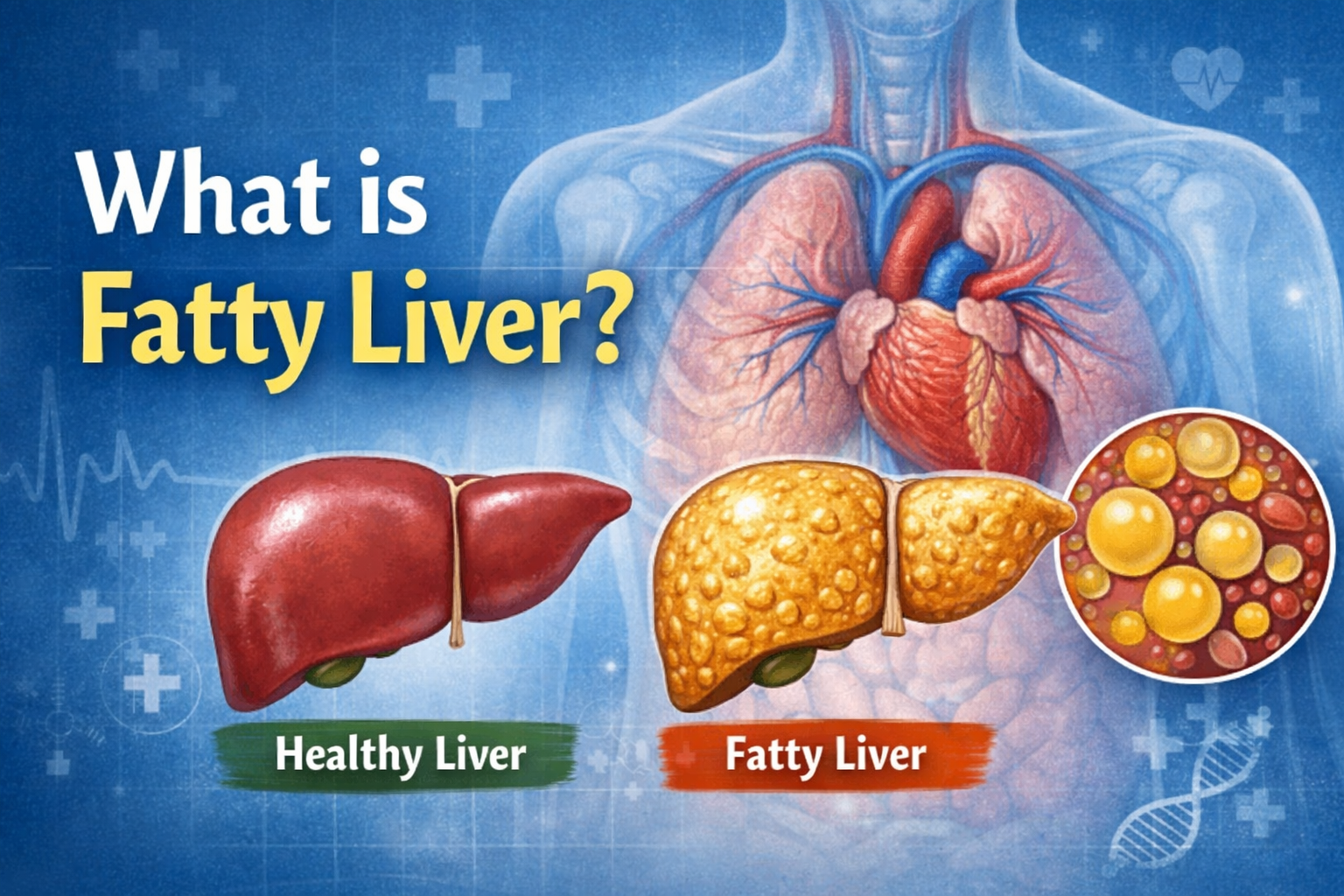
Understanding Fatty Liver Disease
Fatty liver disease, medically known as hepatic steatosis, is a condition characterized by the excessive accumulation of fat in liver cells. While it’s normal for the liver to contain some fat, problems arise when fat makes up more than 5-10% of the liver’s weight.
Your liver is one of the hardest-working organs in your body, performing over 500 vital functions including filtering toxins, producing bile for digestion, storing energy, and regulating blood sugar levels. When excess fat builds up in the liver, it can interfere with these critical functions and potentially lead to serious health complications.
The Two Main Types of Fatty Liver Disease
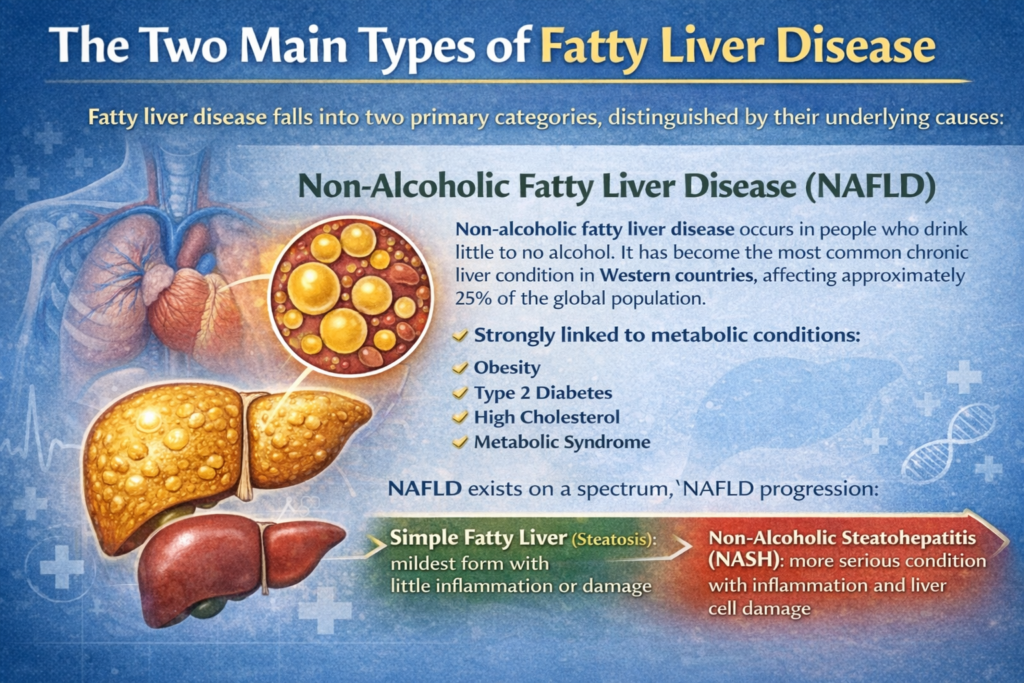
Fatty liver disease falls into two primary categories, distinguished by their underlying causes:
Non-Alcoholic Fatty Liver Disease (NAFLD)
Non-alcoholic fatty liver disease occurs in people who drink little to no alcohol. It has become the most common chronic liver condition in Western countries, affecting approximately 25% of the global population. NAFLD is strongly linked to metabolic conditions such as obesity, type 2 diabetes, high cholesterol, and metabolic syndrome.
NAFLD exists on a spectrum of severity. Simple fatty liver, or steatosis, is the mildest form where fat accumulates in the liver but causes little inflammation or damage. However, in some people, NAFLD can progress to a more serious condition called non-alcoholic steatohepatitis (NASH), where inflammation and liver cell damage occur alongside fat accumulation.
Alcoholic Fatty Liver Disease (AFLD)
Alcoholic fatty liver disease develops as a result of heavy alcohol consumption over time. When you drink alcohol, your liver works to break it down, but this process generates harmful substances that can damage liver cells, promote inflammation, and encourage fat accumulation.
The good news is that alcoholic fatty liver disease is often reversible in its early stages if you stop drinking alcohol completely. However, continued alcohol consumption can lead to more severe liver damage, including alcoholic hepatitis and cirrhosis.
What Causes Fatty Liver Disease?
The development of fatty liver disease involves complex metabolic processes, but several key factors contribute to fat accumulation in the liver:
Metabolic Factors
Insulin resistance plays a central role in the development of NAFLD. When your cells become resistant to insulin, your body produces more insulin to compensate. This excess insulin promotes fat storage in the liver and prevents the breakdown of existing fat stores.
Obesity, particularly excess abdominal fat, significantly increases the risk of fatty liver disease. The fat cells in your abdomen release inflammatory substances and free fatty acids that travel to the liver, contributing to fat buildup and inflammation.
Dietary Influences
A diet high in refined carbohydrates, sugar, and especially fructose can contribute to fatty liver disease. When you consume more calories than your body needs, particularly from sugary foods and beverages, your liver converts these excess calories into fat for storage.
Trans fats and saturated fats, commonly found in processed and fried foods, can also promote liver fat accumulation and inflammation. Additionally, a diet low in fiber and antioxidants deprives your liver of the nutrients it needs to function optimally and protect itself from damage.
Other Contributing Factors
Certain medical conditions increase the risk of developing fatty liver disease. These include type 2 diabetes, high cholesterol and triglycerides, polycystic ovary syndrome (PCOS), hypothyroidism, and sleep apnea.
Some medications can also contribute to fatty liver disease, including corticosteroids, some cancer medications, and certain heart medications. Rapid weight loss, particularly from crash dieting or bariatric surgery, can temporarily worsen fatty liver disease before it improves.
Genetic factors also play a role, with certain genetic variations making some people more susceptible to developing fatty liver disease even with minimal risk factors.
Recognizing the Symptoms
One of the most challenging aspects of fatty liver disease is that it often produces no symptoms in its early stages, earning it the nickname “silent liver disease.” Many people discover they have fatty liver disease only during routine blood tests or imaging studies performed for other reasons.
When symptoms do occur, they are often vague and nonspecific. You might experience persistent fatigue or weakness that doesn’t improve with rest. Some people notice a dull or aching sensation in the upper right abdomen where the liver is located. Unexplained weight loss or a general feeling of being unwell can also occur.
As the disease progresses to more advanced stages, additional symptoms may develop. These can include yellowing of the skin and eyes (jaundice), swelling in the legs and abdomen, easy bruising or bleeding, and confusion or difficulty concentrating.
It’s important to understand that the absence of symptoms doesn’t mean your liver is healthy. Regular medical check-ups and screening are essential, especially if you have risk factors for fatty liver disease.
How is Fatty Liver Disease Diagnosed?
Diagnosing fatty liver disease typically involves several steps and different types of tests:
Blood Tests
Liver function tests measure levels of liver enzymes, particularly ALT (alanine aminotransferase) and AST (aspartate aminotransferase). Elevated levels can indicate liver inflammation or damage, though some people with fatty liver disease have normal enzyme levels.
Your doctor may also order tests to check for other conditions associated with fatty liver disease, such as diabetes screening (fasting glucose and HbA1c) and lipid panel (cholesterol and triglycerides).
Imaging Studies
Ultrasound is often the first imaging test used to detect fatty liver disease. It’s non-invasive, widely available, and can identify fat in the liver, though it may miss mild cases.
More advanced imaging techniques provide additional information. CT scans and MRI can measure the amount of fat in the liver more precisely. A specialized MRI technique called MRI-PDFF (proton density fat fraction) is considered the gold standard for quantifying liver fat non-invasively.
FibroScan, also known as transient elastography, uses sound waves to measure liver stiffness, which can indicate the presence of scarring or fibrosis. This painless test takes just a few minutes and provides immediate results.
Liver Biopsy
In some cases, particularly when NASH or significant fibrosis is suspected, your doctor may recommend a liver biopsy. This involves taking a small sample of liver tissue with a needle for examination under a microscope. While a biopsy is the most definitive way to diagnose NASH and assess the degree of liver damage, it’s invasive and carries small risks, so it’s not performed on everyone with suspected fatty liver disease.
The Progression of Fatty Liver Disease
Understanding how fatty liver disease can progress helps emphasize the importance of early intervention:
Simple fatty liver (steatosis) is the first stage, where fat accumulates but causes minimal inflammation or damage. Many people remain at this stage indefinitely, especially with lifestyle modifications.
Non-alcoholic steatohepatitis (NASH) develops when inflammation and liver cell damage occur alongside fat accumulation. Approximately 20% of people with NAFLD progress to NASH, which carries a higher risk of further complications.
Fibrosis represents the development of scar tissue in the liver as it attempts to repair itself from ongoing inflammation and damage. Early fibrosis may be reversible with appropriate treatment and lifestyle changes.
Cirrhosis is advanced scarring where scar tissue replaces healthy liver tissue extensively. At this stage, liver damage is generally irreversible and can lead to liver failure. People with cirrhosis face an increased risk of liver cancer.
The good news is that progression isn’t inevitable. With early detection and appropriate intervention, particularly lifestyle modifications, many people can halt or even reverse fatty liver disease before it advances to more serious stages.
Treatment and Management
Currently, there are no FDA-approved medications specifically for treating fatty liver disease, making lifestyle modifications the cornerstone of treatment:
Weight Loss
If you’re overweight or obese, losing 7-10% of your body weight can significantly reduce liver fat, inflammation, and even fibrosis. The key is gradual, sustainable weight loss through a combination of healthy eating and increased physical activity. Aim to lose 1-2 pounds per week, as rapid weight loss can temporarily worsen liver inflammation.
Dietary Changes
Adopting a Mediterranean-style diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats has shown particular benefit for fatty liver disease. Focus on reducing your intake of refined carbohydrates, added sugars, and saturated fats.
Limit or eliminate sugar-sweetened beverages, which are a major source of excess fructose. Reduce consumption of red and processed meats, and choose fish, poultry, and plant-based protein sources instead. Increase your fiber intake through whole grains, legumes, fruits, and vegetables.
Regular Exercise
Physical activity helps reduce liver fat even without significant weight loss. Aim for at least 150 minutes of moderate-intensity aerobic exercise per week, such as brisk walking, swimming, or cycling. Include resistance training exercises at least twice a week to build muscle and improve insulin sensitivity.
Managing Associated Conditions
If you have diabetes, maintaining good blood sugar control is crucial for managing fatty liver disease. Work with your healthcare provider to optimize your diabetes medications and monitoring.
For high cholesterol and triglycerides, dietary changes and medications if needed can help reduce liver fat. If you have high blood pressure, keeping it well-controlled reduces stress on your liver and cardiovascular system.
Avoiding Harmful Substances
Limit or eliminate alcohol consumption, even if you have NAFLD rather than alcoholic fatty liver disease. Avoid unnecessary medications and supplements that can stress your liver. Always consult your doctor before starting new medications or supplements.
Prevention: Your Best Defense
Preventing fatty liver disease is much easier than treating it. Here are key strategies:
Maintain a healthy weight through balanced eating and regular physical activity. Eat a nutrient-dense diet rich in whole foods while limiting processed foods, added sugars, and unhealthy fats.
Stay physically active with at least 150 minutes of moderate exercise weekly. Limit alcohol consumption to recommended guidelines or avoid it entirely if you’re at risk.
Manage chronic conditions like diabetes, high cholesterol, and high blood pressure effectively. Get regular health check-ups, including blood tests to monitor liver function, especially if you have risk factors.
When to See a Doctor
You should consult a healthcare provider if you experience persistent fatigue, abdominal discomfort, or unexplained weight changes. If you have risk factors such as obesity, diabetes, or metabolic syndrome, ask about fatty liver screening even without symptoms.
Regular monitoring is essential if you’ve been diagnosed with fatty liver disease. Your doctor can assess disease progression and adjust your treatment plan as needed.
Living with Fatty Liver Disease
A diagnosis of fatty liver disease isn’t a life sentence. Many people successfully manage or even reverse the condition through dedicated lifestyle changes. The key is consistency and patience – improvements in liver health typically occur gradually over months to years.
Focus on sustainable changes rather than quick fixes. Build a support system of healthcare providers, family, and friends who can encourage your healthy lifestyle journey. Stay informed about your condition and actively participate in your care decisions.
Remember that small, consistent changes add up over time. Whether it’s choosing water instead of soda, taking a daily walk, or preparing more meals at home, each positive choice supports your liver health.
Conclusion
Fatty liver disease is a serious but often reversible condition that affects millions of people worldwide. While it may not cause symptoms in its early stages, understanding your risk factors and taking proactive steps to protect your liver health is crucial.
Through healthy lifestyle choices – maintaining a healthy weight, eating a balanced diet, exercising regularly, and managing associated health conditions – you can significantly reduce your risk of developing fatty liver disease or prevent its progression if you’ve already been diagnosed.
If you’re concerned about fatty liver disease, don’t wait for symptoms to appear. Talk to your healthcare provider about screening, especially if you have risk factors. Early detection and intervention offer the best opportunity for maintaining a healthy liver and preventing serious complications.
Your liver is remarkably resilient and capable of healing when given the right support. By taking action today, you’re investing in your long-term health and well-being.
Medical Disclaimer: This article is for informational purposes only and is not intended as medical advice. Always consult with a qualified healthcare provider for diagnosis and treatment of fatty liver disease or any other medical condition. Individual circumstances vary, and treatment should be personalized based on your specific health needs.









3 Comments